Chronic pain affects many people every day. It could be because of age, injury, and underlying illnesses. The brain signals your body through the nervous system about your pain, and once you’ve taken measures to address it, like taking an oral medication, the pain should subside. But if the pain comes and goes and persists for more than three to six months, doctors define it as chronic pain. In 2019, 26% of the US adult population aged 45 to 64 years old suffered from chronic pain. This kind of ailment affects their day-to-day life, livelihood, and, most importantly, mental health. Read about Epidural Injections
Chronic pain can be the result of the following conditions:
- nerve damage
- back pain
- neck pain
- leg pain
- migraine
- arthritis
- sciatica
- herniated disc
The best procedure for LSS patients is still the MILD procedure. It basically has the same low level of risk as epidural injections, but the difference is that it has a lasting effect.
In recent years steroid injections have shown excellent results in addressing chronic pain for patients who have been suffering from it.
What is Steroid Epidural Injection?
An epidural steroid injection (ESI) is administering pain medicine quickly into the body with a syringe.
Epidurals are often used during labor and childbirth and some types of surgery to administer anesthesia effectively.
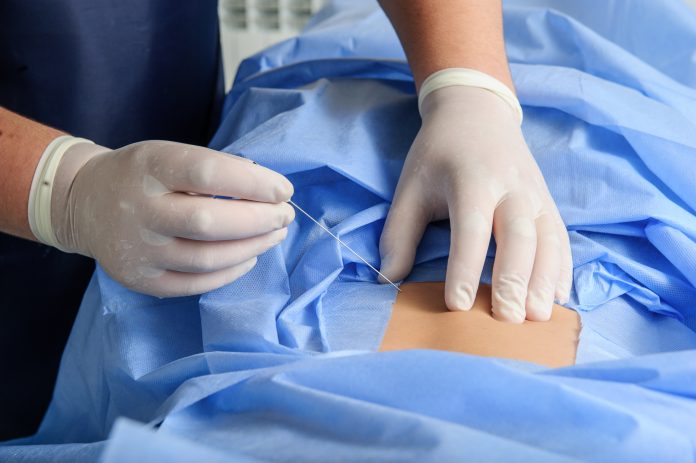
The patient may be asked to lie on their belly or sit in a fetal position to administer the steroid. A local anesthetic to numb the skin will be placed, and a needle will be inserted with the guidance of an x-ray called fluoroscopy to reach the epidural space.
After the procedure, the patient may be sent home but will be advised to limit physical activities for a day or two. The pain relief may be felt immediately because of the local anesthetic, but the effects of the steroids will be noticed after three to five days and can last for months. If you want to know more about steroids for epidural injections, you may visit this recommended site.
What Are Common Types Of Steroids For Epidural Injections?
Steroids, short for corticosteroids, are synthetic anti-inflammatory drugs. They resemble the hormone cortisol that your body naturally produces.
Cortisol is your body’s built-in warning system. It is released when you’re feeling stressed or when you’re in pain. Cortisol plays a vital role in keeping inflammation down, regulating your blood pressure, and controlling your body’s circadian rhythm.
The steroids used in managing pain are different from those athletes use for bodybuilding. Those are anabolic steroids or performance-enhancing drugs, a synthetic version of the hormone testosterone.
Steroids for epidural injections were first used in 1900 in Paris to treat sciatica and back pain, and since then, it has gained popularity as an alternative treatment for chronic pain. To give you an idea, here are the most common steroids used for epidural injections:
1. Dexamethasone
Dexamethasone is used for transforaminal epidural injections to treat radicular pain. Radicular pain is the kind of pain that radiates from your back and hip into your legs through the spine. This often happens when the spinal nerves get pinched or compressed.
Dexamethasone is recommended for chronic pain because of its good analgesic effect and less unfavorable effect on plasma cortisol, blood glucose, and ACTH or adrenocorticotropic hormone.
Herniated discs, scar tissue from prior surgery, and diabetes could be the reasons why your nerves get inflamed and become painful. Not addressing this condition could worsen one’s medical situation and lead to depression.
According to a study, 4mg of dexamethasone at 12 weeks of continuous injections through lumbar transforaminal epidural revealed satisfactory results with no serious adverse side effects noted. Long-term safety and tolerability in patients were also observed.
2. Triamcinolone
Triamcinolone is commonly used in cervical interlaminar epidural injections to address cervical radiculopathy.
Cervical radiculopathy happens when a nerve root in the cervical spine (the neck region of your backbone) becomes inflamed. This results in pain that radiates from the neck into the shoulders and upper extremities. (canadianpharmacy365.net) The range of pain may start with a simple pins-and-needles tingling sensation to a shock-like burning pain.
The most common cause of cervical radiculopathy is a bone spur and spinal degeneration. Long-term suffering from this may eventually lead to paralysis.
Triamcinolone injection is also used to treat certain types of arthritis, allergies, skin diseases, and gout. However, the injection route is not epidural or intravenous for these ailments but could be administered intramuscularly, intradermally, or intraarticularly.
3. Methylprednisolone
Methylprednisolone is used in transforaminal epidural steroid injection or TFESI.
TFESI is made to treat lumbosacral radicular pain or lumbar radiculopathy, which occurs when a spinal nerve is compressed or inflamed. The pain is usually felt in the lower extremity, down the back of the thigh and calf into the foot. (https://morrisvillecathospital.com/)
In layman’s terms, this is referred to as sciatica. The pain may be constant or intermittent. The burning and shooting pain may be more severe on the leg than on the back, and aside from the pain, weakness on the affected leg may also occur. Because of this, patients may have limited mobility because sitting and walking could aggravate the pain.
4. Betamethasone
Betamethasone as an epidural injection is used to treat osteoarthritis, gouty arthritis, bursitis, and rheumatoid arthritis. Improvement of pain can be felt for as long as four months, and better outcomes are seen for earlier treatments.
What are the risks of an ESI?
Generally, you will not encounter any problems after having an ESI, but side effects may include:
- Nausea
- Headache
- Dizziness
- Steroid flush – warmth felt on the face and chest that may occur for several days
Serious complications are rare, but some of them could be:
- Infection
- Paralysis
- Nerve damage
- Bleeding
- Allergic reaction
Conclusion
Non-surgical management of pain is an option many people prefer. The minimally invasive procedure could mean that they could return to their routine at the soonest possible time.
Though ESI could greatly help manage the pain of several conditions, many health specialists also recommend integrating physical therapy to maximize the benefits of ESI. For better results, always consult your trusted healthcare professional so that any treatment and therapy you may want to try will not exacerbate the pain and your condition.